Nanoparticle Therapy – An Emerging Cancer Treatment
5 Min Read
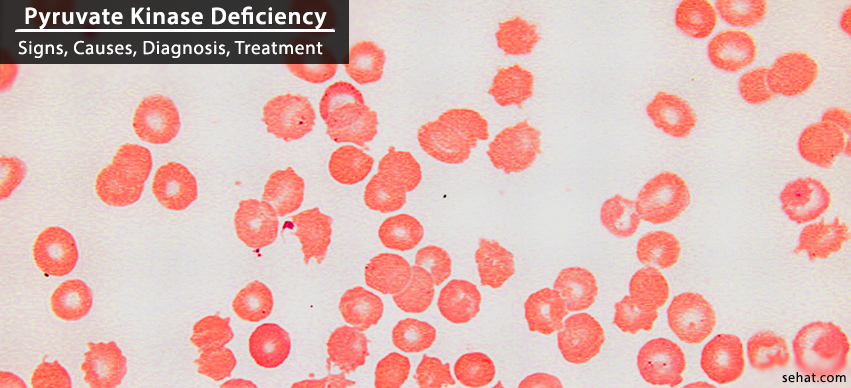
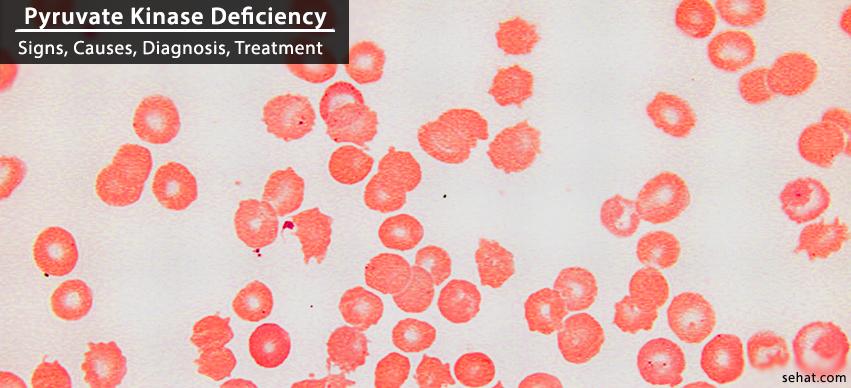
Pyruvate kinase deficiency is one such inherited disease that directly affects red blood cells (RBC’s) carrying oxygen to body tissues. As such, people suffering from this particular kind of disorder succumb to a condition known as chronic hemolytic anemia where the red blood cells undergo hemolysis and are broken down, resulting in anemia.
Reportedly, Pyruvate kinase deficiency happens to be one of the most commonly inherited cause for nonspherocytic hemolytic anemia and affects more than 500 families on an average, across all ethnic groups. Also, medical researchers believe that it's underdiagnosed as it is mostly not identified in mild cases. The prevalence of the disease can be estimated as 1 out of a total of 20000 people across the European subcontinent being more popular around the Amish settlement of Pennsylvania.
In the case of hereditary nonspherocytic hemolytic anemia, the red blood cells fail to assume their spherical shape akin to other types of hemolytic anemia. Chronic hemolytic anemia usually results in:
Individuals suffering from pyruvate kinase deficiency as well as hemolytic anemia along with other complications usually show mild to severe symptoms. However, in some instances, affected people tend to show a few to no signs at all. When affected during infancy, such a condition can be life-threatening and might require blood transfusions at regular intervals to survive. The symptoms tend to get worse during pregnancy or any kinds of infection.
Pyruvate kinase deficiency is mainly caused due to PKLR gene mutation. The PKLR gene stays active within the liver and within red blood cells where it functions to develop an enzyme known as pyruvate kinase. The enzyme plays a vital role in an energy producing process termed as glycolysis, which involves breaking down of glucose into two molecules of ATP, which acts as a power source for all living cells. The PKLR gene mutation leads to a reduction of enzyme function, which further affects ATP in RBC’s and enhanced levels of other molecules earlier generated by glycolysis. Any such abnormal RBC’s are stored in the spleen which eventually gets destroyed, leading to hemolytic anemia and further an enlarged spleen.
The shortage of RBC’s carrying oxygen across the body is what causes fatigue, pallor, and dyspnea. Iron, along with other molecule known as bilirubin, is released following the destruction of red blood cells. Thus, any excess amount of bilirubin present in the blood causes jaundice as well as gallstone. Pyruvate kinase deficiency can also take place due to after effect of other blood-related diseases, leukemia for instance. Such cases are known as secondary pyruvate kinase deficiency, and no inheritance pattern is observed. The inheritance pattern in Pyruvate kinase deficiency occurs due to the autosomal recessive pattern, where both the copies of the gene in each cell show mutations. Hence, the parents of an individual who shows such recessive condition each carry a copy of the gene that is mutated. However, generally, they do not depict any sign or symptom of the so-called condition.
There are equipped labs offering clinical testing for Pyruvate kinase deficiency disease to help affected families and support them in any decision related to medical care. To facilitate diagnosis, it is recommended that you talk to a genetic professional to get an ally about your medical options.
In case of a mild case of pyruvate kinase deficiency, there is usually no specific treatment plan that is available or recommended. However, people suffering from anemia might require blood transfusions. For many newborns, terrible jaundice case is being witnessed to which the attending professional might exchange transfusion. In extreme cases, the spleen may be required to be moved surgically which in turn may help counteract the destruction of RBC's.
However, such an action plan is not recommended in case of a minor. With very small children, this is usually delayed, offering ample chance for immune systems to turn mature. Other forms of treatment are symptomatic as well as supportive in nature. Anyone who underwent splenectomy should receive the pneumococcal vaccine at regular intervals as directed by the attending doctor.
There is a natural way the body tries to treat this disease by increasing the production of Erythrocyte, known as reticulocytosis. This precisely because reticulocytes are nothing but red blood cells which are immature and still have mitochondria to produce ATP through oxidative phosphorylation. A Mature erythrocyte usually lacks nucleus as well as mitochondria. Hence, without the nucleus, they are not in state synthesizing proteins. So, anything happens to their pyruvate kinase, they are left vulnerable without any chance to generate any replacement enzymes in their life cycle. Also, without the presence of mitochondria, erythrocytes dote heavily upon anaerobic generation of ATP that takes place in glycolysis for all kinds of energy generation.
Pyruvate kinase deficiency is one such disease that shows variable prognosis. While some people might show few to almost no symptoms at all, others might have severe symptoms. Affected individuals who have mild to moderate symptoms reportedly do well in the long term. On the other hand, others who depict severe symptoms are generally symptomatic during their early childhood. As the individuals grow from being a child, the condition becomes typically better owing to the growth of immunity systems. However, there are certain cases, where people tend to develop certain complications like gallstones or might experience a stroke. Also, following a splenectomy, there is a strong chance of several difficulties due to pneumococcal diseases.
In splenectomy, there is no stopping the erythrocytes and its destruction, but it helps to increase reticulocytes and its amount within the body. As such, a majority of hemolysis takes place when reticulocytes remain trapped within the hypoxic environment resign within the spleen. It dramatically helps to reduce severe conditions of, and hence, there occurs a need for blood transfusion.