How Communities Are Changing the Way We Think About Aging in..
8 Min Read
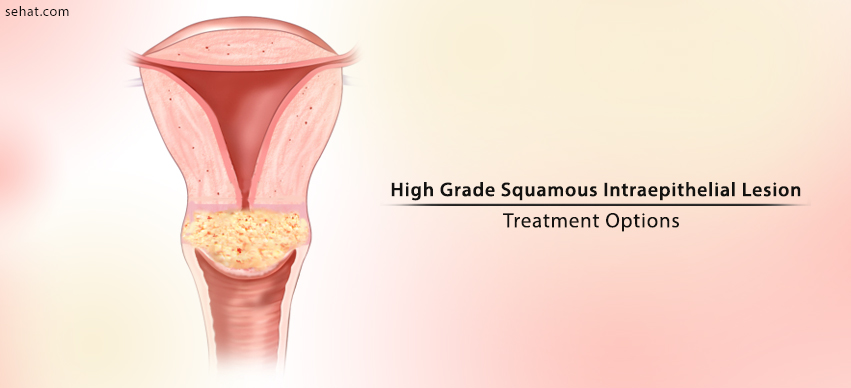
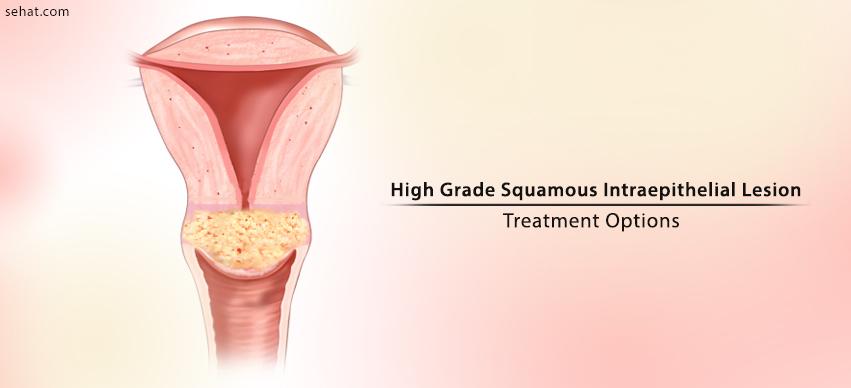
High-Grade Squamous intraepithelial lesion (HSIL) is the abnormality of the squamous cell caused by the Human Papillomavirus. The condition is more commonly found in young and sexually active females. The risk of high grade squamous intraepithelial lesion decreases till menopause and some studies indicate increased risk post-menopause. The condition is also categorized as moderate or severe dysplasia. Most women do not experience high grade squamous intraepithelial lesion symptoms.
In 2014, the World Health Organization adopted the terminology HSIL which encompasses CIN (Cervical Intraepithelial Neoplasia) 1, CIN 2, carcinoma in situ and dysplasia. High grade squamous intraepithelial lesion (CIN3) is characterized by the occurrence of abnormal cells in more than two-thirds of the whole thickness of the cervical epithelium.
The condition is generally diagnosed with the Pap smear test. The procedure includes collecting the cells for analysis from the cervix. The cervix is that part of the uterus which gets extended into the vagina. The cells, as well as mucus, helps in determining the presence of HPV infection.
If the report comes positive for HSIL, it indicates the presence of abnormal cells with higher differences in shape and size as compared to normal cells. High-grade is the designation given due to the presence of precancerous cells having a high risk of transformation to invasive cancer.
Human Papillomavirus (HPV) is the cause of HSIL. Human papillomavirus infects the genital tract lining of women. It is a common infection and spread through sexual contact. In most cases, the infection occurs without any symptoms and does not require any treatment. However, if the infection persists for a longer period, the risk of development of HSIL and cancer increases. The risk of infection increases with an increase in the number of sexual partners.
To get rid of high grade squamous intraepithelial lesions, various treatment options are available. The option chosen depends upon the severity of the condition and the changes in the morphology of the cervical tissue. The treatment options include the destruction of the abnormal cells, technically known as ablative therapy, and removal of the affected tissues also known as excisional therapy.
In ablative treatment, the abnormal cells are removed from the cervix. Most common techniques used for this treatment are Cryotherapy and Laser Ablation.
This treatment is generally recommended in case of relatively smaller lesions and when the lesions are not extended into the endocervical canal. Further, for cryotherapy to be an appropriate option, there should not be any invasive condition and the complete lesion should be in the reach of the surgeon. Before starting the procedure, a patient consent form gets signed from the patient which indicates, among other information, the side effects associated with the surgery. The patient is advised to lie in the dorsal lithotomy position. A vaginal speculum is inserted and a vaginal side wall detractor is used to clearly visualize the lesion. A probe tip is selected as per the size of the lesion and it should produce at least 20 pounds per square inch of pressure. The probe tip is placed tightly on the lesion and the cycles of freeze-thaw-freeze are initiated. According to WHO recommendation, the cycle should be of 3-minute freeze, 5-minute thaw, and 3-minute thaw. Side effects of cryotherapy include menstrual like cramps, vaginal bleeding and vaginal discharge that may last for around 1 month.
As this treatment includes the use of Laser, proper safety guidelines should be followed while performing this technique. Protective eyewear should be used and the blackened speculum should be used to prevent the damage of healthy tissues if in case any beam gets misdirected. Using colposcopy, a CO2 laser is directed on the lesion. Water present in the cells gets evaporated due to the energy created by Laser beam and the cells get destroyed.
This treatment is used to remove the tissues from the cervix. Such treatment is advised when there are concerns of invasive disease and in case of recurrence of dysplasia after the previous ablative of excisional treatment.
Prior to treatment, the patient is provided with analgesic and anti-inflammatory medicine to reduce pain. The patient is placed in the dorsal lithotomy position. Vaginal wall detractor may be used to clearly view and get access to the cervix. For delineation of the zone and to provide antisepsis to the region, Iodine solution (Lugol solution) is used. A loop of appropriate size is used to remove the complete transformation zone. For anesthesia and to reduce the risk of bleeding, local anesthetics such as lidocaine is mixed with other drugs such as vasopressin. For removing the lesions that have been extended in the endocervical region, cowboy hat technique is used.
Cold-knife conization or laser conization may be used to remove the lesions. Prior to LEEP, Cold knife conization was mainly used to remove lesions. However, because of its side effects this technique, it is reserved only for those cases where LEEP is not viable. A speculum is inserted into the cervix and with the help of a scalpel, a cone-shaped specimen is removed. Lugol solution and local anesthetic mixed with vasopressin are used during treatment. The side effects of Cold Knife conization are bleeding, infection, and cervix stenosis.