How Communities Are Changing the Way We Think About Aging in..
8 Min Read
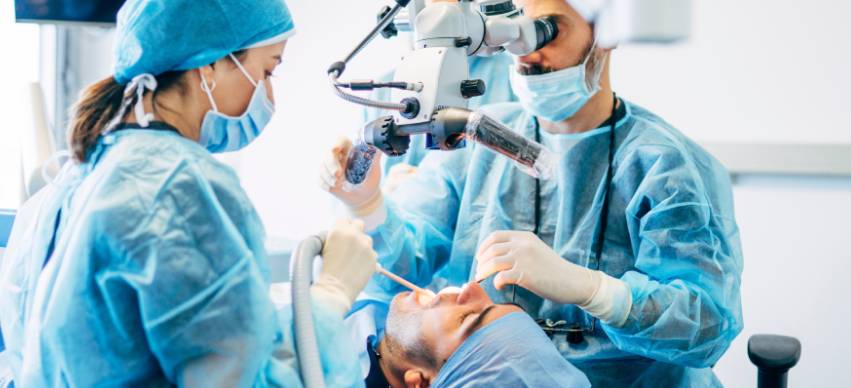
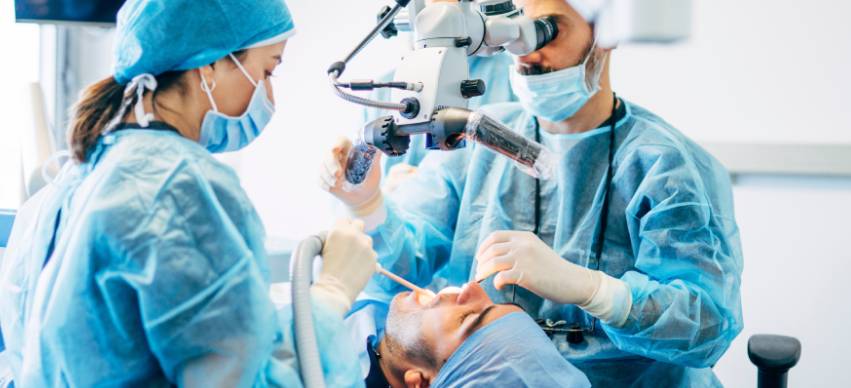
Oral surgery consists of surgical operations on oral structures, including jaws, teeth, and gums. Some forms of oral surgery include placing implants, teeth extraction, jaw surgery, and gum grafts. This type of surgery can be performed by either a periodontist or an oral and maxillofacial surgeon. These professionals are specially trained in performing oral surgery.
In addition, oral surgery can be performed for decayed, broken, or impacted teeth, sleep apnea, and bone loss in the jaws.
If you suspect that you’re having any of the above issues, ensure that you consult a dentist to receive a diagnosis. You can go here if you need help finding professional and reputable dentists for a wide range of dental services.
You must get a physical examination of the mouth and all other surrounding structures to determine if you’ll need oral surgery. A dentist or oral surgeon must conduct the examination.
A thorough examination of the teeth, gums, tongue, and jaw can provide a diagnosis for several oral issues that might require surgery. You may also be asked to undergo imaging tests such as X-rays, and computerized tomography (CT) scans to look at the bone structure in the mouth.
Additionally, a biopsy may be required depending on the assessed condition. A tiny tissue sample is retrieved and studied under a microscope in a biopsy. The results of the biopsy can help determine what the issue could be and the necessary oral surgery. Likewise, a diagnosis can be made using blood tests or genetic testing.
Oral surgery is not a one-size-fits-all. There are several types of oral surgery performed by oral surgeons, such as the following:
Tooth removal is the most common oral surgery. Your dentist can recommend getting a tooth extraction for the following issues:
A tooth extraction may also be necessary for preparation to input dentures or any other prosthetic device. While a dentist would prioritize saving your natural teeth, an extraction might be required in extreme circumstances to conserve oral health. You can also be subjected to tooth extraction in preparation to input dentures or any other prosthetic device.
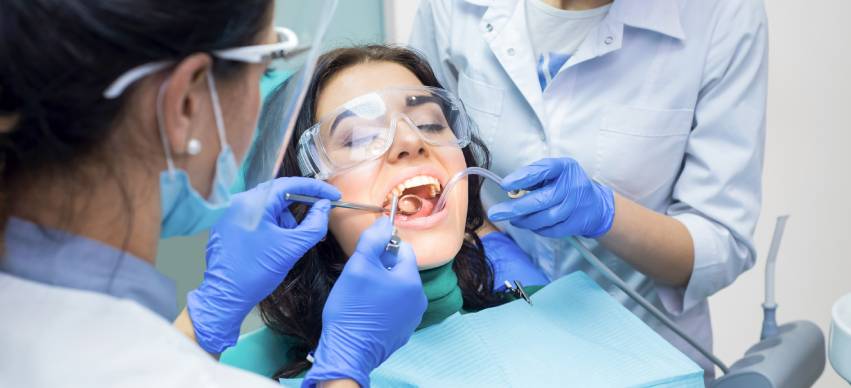
Extracting wisdom teeth, meanwhile, is usually the best option. Wisdom teeth, or third molars, typically grow at an angle that can impact other teeth. This may cause pain, infection, or tooth decay, thus making extraction a better choice for oral health.
Your dentist can recommend getting dental implants after tooth extraction. Ideally, an implant is a long-lasting replacement option for teeth in the form of small threaded posts. There are several benefits and drawbacks of getting dental implants, and you should consider all these when deciding to get the procedure.
Dental implants are often made of medical-grade titanium or zirconia and placed into the jaw to restore missing teeth roots. When the implants are healed, your dentist can restore them by including dental crowns, bridges, and dentures.
Dental implants can also include endosteal implants embedded into the jawbone and the subperiosteal under the gum and over the jawbone. Your dentist should explain the type of implant you’re getting and any impact it might have on your oral health.
If you have bone loss in your jaw, the dentist might recommend getting a dental bone graft. You can suffer from bone loss for many reasons. First, the roots in your natural teeth stimulate the nerves in the jaw. The stimulation sends signals to the brain for nutrients for the jaw to keep it strong and healthy.
In instances where a tooth is missing, there’ll be no roots to stimulate the nerves, which can cause bone deterioration in that area. When you receive a dental bone graft, it’ll reinstate the volume and density of the jawbone. This helps when getting dental implants later on.
You can also receive a dental bone graft for advanced gum disease during periodontal surgery. This is because the bones around the teeth could be eroded. The purpose of a bone graft is to offer a strong foundation for strong and healthy teeth.
In cases of severe gum disease, your dentist can recommend getting periodontal surgery as a form of treatment. You’ll get incisions along the gum line for the procedure, with the tissue temporarily moving away from the teeth. This allows the surgeon to clean the teeth roots and flush any plaque and bacteria that might have amassed on the gums. The final step is to reposition and suture the gum tissue.
With gum recession, the dentist might recommend getting a gum graft. In this case, the surgeon uses donor tissue to reinforce the area affected by tissue loss. The donor tissue can be from the roof of your mouth or acquired from a certified tissue bank.
You may be diagnosed with obstructive sleep apnea if the tissues in your throat pull back and obstruct the airways. Oral surgery may be the best option if oral appliance therapy can’t treat the obstruction.
Once you’ve been diagnosed with an oral issue that requires surgery, you’ll have to start prepping for the procedure. Preparations for surgery can differ depending on the problem being treated and the purpose of the surgery. Nonetheless, it’d help if you prioritized taking care of your teeth at all times, especially in between checkups and prepping for the procedure.
You might also need a consultation with your surgeon to discuss the diagnosis, operative procedure, and expected results. At this point, you can voice any concerns about the procedure. The surgeon can also explain all the steps that’ll be taken during the procedure.
Some of the factors to consider in preparation for oral surgery include the following:
Ensure you consult the oral surgeon on what’s expected of you while preparing for the surgery. You should respond to all the questions asked by the surgeon and disclose all the information necessary, including any medication you might be on.
On the day of the oral surgery, you’ll go through several preoperative procedures. These procedures can be different depending on the anesthesia you’ll be using. The following preoperative procedures can be performed:
Once you’re ready and the anesthesia has been properly administered, the surgeon will proceed with the procedure. The oral procedure can either be open, endoscopic, or minimally invasive. It can also be classified as either constructive or cosmetic. properly administered, the surgeon will proceed with the procedure. The oral procedure can either be open, endoscopic, or minimally invasive. It can also be classified as either constructive or cosmetic.
The time taken for the surgery depends on the procedure being done. If you’re getting a tooth extraction, it can take about 30 minutes. An extensive procedure can take more time.
Upon completion of the oral surgery, you’ll be placed in the recovery room for observation as the anesthesia wears off. The surgeon can let you leave the facility once they deem it safe. You’ll be required to care for the wound by taking pain medication to manage any post-operative pain you may experience and oral antibiotics to prevent infection
Ensure that you follow all the post-operative guidelines to aid proper healing and reduce the possibility of bleeding and getting an infection.
Your recovery from oral surgery depends on several factors, including adhering to the post-operative guidelines. In addition, your recovery time also depends on the type of oral surgery you get. An invasive surgery will most likely have a longer recovery time than a non-invasive procedure.
You can also enhance your recovery by adhering to the recommended dietary plan. For instance, if you’ve been asked to take soft foods and liquid meals, ensure they are nutritious. This ensures that the surgical site won’t be irritated.
Nonetheless, you must inform your oral surgeon or dentist if you experience any issues such as pain or bleeding. This is crucial in detecting any complications early and initiating an intervention.
Oral health directly impacts your general health. This includes all structures in your mouth, including your teeth, gums and jaw. Thus, it’d help if you visited your dentist regularly for checkups which can help detect issues early and avoid oral surgery. But if you need oral surgery, above is an outline of the basics of what you need to know to prepare for the procedure.